Foods to Avoid With Uveitis and Why They Matter
Uveitis is an eye disease linked to inflammation inside the eye, and it can affect vision in ways that feel unpredictable at first. The condition involves the middle layer of the eye, including the ciliary body, and may also influence other tissues nearby. Because uveitis affects structures responsible for nourishment and focus, even small changes can feel noticeable. Alongside medical care, everyday choices such as diet can play a vital role in how symptoms behave over time.
Understanding Uveitis and Inflammation
Uveitis is a medical condition driven by inflammation that can involve delicate structures inside the eye, which helps explain why symptoms vary from one person to the next.
 How Uveitis Develops Inside the Eye
How Uveitis Develops Inside the Eye
The inflammation associated with uveitis often begins within the middle layer, where blood vessels supply nutrients to the eye. When these vessels become irritated, fluid movement and circulation can shift. This process may influence the optic nerve and nearby structures that support vision. Over time, ongoing irritation increases the risk of complications if left unmanaged.
Why the Immune Response Matters
Your immune system plays a central role in how uveitis develops and behaves. In some cases, the condition is linked with autoimmune diseases or inflammatory diseases such as rheumatoid arthritis. When immune activity becomes misdirected, inflammation can persist beyond its useful purpose. This helps explain why uveitis can appear alongside other inflammatory conditions.
Recognising Symptoms Early
Symptoms may appear gradually or arrive without much warning. Common symptoms include eye redness, light sensitivity, blurred vision, and discomfort that affects one or both eyes. These symptoms of uveitis can fluctuate, which sometimes delays recognition. Paying attention to changes supports early discussion with an eye doctor.
Factors That Influence Severity
Several lifestyle factors and elements of your medical history can influence how strongly uveitis presents. In modern lifestyles, diet patterns and stress may contribute to inflammatory responses. When inflammation continues unchecked, there is a greater risk of vision loss or permanent damage. Early awareness helps prevent complications linked to prolonged activity.
Foods to Avoid With Uveitis
Diet does not replace care, but certain foods can aggravate inflammation and make uveitis symptoms harder to manage.
Processed and Red Meats
Red and processed meats often contain additives and fats that can trigger inflammation. Diets high in these foods may place extra strain on blood vessels already affected by inflammatory activity. Regular intake has been linked with flare-ups in some uveitis patients. Reducing frequency can support steadier symptom patterns.
High-Sugar and Refined Carbohydrates
Sugary snacks, refined carbohydrates, and white bread can contribute to sharp blood sugar changes. These fluctuations may worsen inflammatory responses in the body. Over time, diets high in refined foods may affect overall health and recovery patterns. Moderation can help stabilise energy and inflammatory load.
Unhealthy Fats and Excess Salt
Unhealthy fats such as trans fats and saturated fats are common in processed food. These fats may contribute to inflammation and water retention, which can increase pressure in sensitive tissues. High-sodium foods can further complicate fluid balance. Choosing alternatives helps reduce unnecessary strain.
Dairy and Certain Plant Foods
Some find that dairy products or nightshade vegetables aggravate symptoms, although responses vary. These foods may influence inflammation levels in susceptible individuals. Awareness helps you notice patterns linked to flare-ups. Adjustments should be gradual and considered.
The Broader Dietary Pattern
A modern dietary pattern often includes inflammation-causing foods consumed regularly. When meals are built around convenience and excessive processing, inflammatory responses can intensify. Understanding foods to avoid with uveitis helps you make informed decisions without drastic restriction. Small changes often feel more sustainable.
Supporting Uveitis Management Through Diet
Dietary choices work alongside medical treatment to support stability and comfort during recovery.
Focusing on Anti-Inflammatory Choices

Over time, repeated exposure to supportive foods can influence how inflammation behaves day to day. You may notice fewer fluctuations in comfort when meals remain steady and predictable. This approach works well when viewed as a long-term pattern rather than a short-term adjustment.
Nutrients That Support Eye Function
Certain nutrients play supportive roles in eye health. Vitamin C and vitamin E contribute to cellular protection, while zinc oxide supports normal tissue processes. Including citrus fruits and a diet rich in varied nutrients supports overall health. These nutrients complement other care strategies.
When nutrient intake is inconsistent, recovery can feel less settled. You may find that balanced intake supports steadier visual comfort during demanding days. Nutrients work gradually, so benefits often build over time rather than appearing suddenly.
Choosing Stable Carbohydrates
Complex carbohydrates such as brown rice and other whole grains provide steadier energy. These foods support metabolic balance and reduce rapid spikes that can influence inflammation. A stable energy pattern supports managing uveitis over time. Balance helps maintain daily comfort.
Refined carbohydrates can sometimes leave energy feeling uneven. That fluctuation may coincide with changes in eye comfort or fatigue. Choosing slower-digesting options supports consistency across daily routines.
Working With Your Care Team
Diet adjustments should align with advice from your eye doctor and broader care team. Eye drops and other prescribed approaches address active inflammation directly. Dietary changes support these measures without replacing them. Open discussion with your eye doctor helps align expectations.
Clear communication helps avoid conflicting adjustments. You may benefit from reviewing dietary changes during follow-up visits. This shared approach supports coordinated care rather than isolated decision-making.
Long-Term Perspective

Long-term patterns often matter more than short-term shifts. You may notice that small, consistent habits feel easier to maintain than strict changes. Over time, this steadiness can support confidence in daily management.
Ongoing Guidance Matters Beyond Dietary Changes
Uveitis can affect vision and comfort in ways that feel disruptive, especially when inflammation persists. Understanding symptoms, recognising how diet interacts with inflammation, and following medical guidance support steadier outcomes. Thoughtful food choices, combined with care, may help reduce strain on the eyes. If you have concerns or notice changes, we are here to help. Please call our clinic at (03) 9070 5753 to arrange a consultation.
Note: Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
References
https://www.nature.com/articles/s41598-023-37062-8
https://my.clevelandclinic.org/health/diseases/14414-uveitis


 How Uveitis Develops Inside the Eye
How Uveitis Develops Inside the Eye




 Extended hours at a computer, tablet, or phone can contribute to eye strain, which may make your
Extended hours at a computer, tablet, or phone can contribute to eye strain, which may make your Comprehensive eye assessments allow an eye doctor to examine your eyes in detail. These tests can detect:
Comprehensive eye assessments allow an eye doctor to examine your eyes in detail. These tests can detect: If you notice ongoing or sudden blurry vision, seeking guidance can help you understand what is contributing to the change and what approaches may support clearer,
If you notice ongoing or sudden blurry vision, seeking guidance can help you understand what is contributing to the change and what approaches may support clearer, 
 Glaucoma
Glaucoma Certain factors increase the likelihood that a person may develop glaucoma:
Certain factors increase the likelihood that a person may develop glaucoma: Understanding how glaucoma is diagnosed helps you take proactive steps towards maintaining eye health. A combination of comprehensive eye exams ensures an accurate glaucoma diagnosis.
Understanding how glaucoma is diagnosed helps you take proactive steps towards maintaining eye health. A combination of comprehensive eye exams ensures an accurate glaucoma diagnosis.

 Recognising the symptoms of vitreous haemorrhage is an important step in
Recognising the symptoms of vitreous haemorrhage is an important step in
 Refractive Errors
Refractive Errors


 Overview of High Blood Pressure
Overview of High Blood Pressure Blood Pressure Levels and Eye Health
Blood Pressure Levels and Eye Health What is ocular hypertension?
What is ocular hypertension?
 If you’re only experiencing blurry vision in one eye, the underlying causes may be different and often more localised to that eye. These can include conditions like cataracts, refractive errors, glaucoma, or macular degeneration.
If you’re only experiencing blurry vision in one eye, the underlying causes may be different and often more localised to that eye. These can include conditions like cataracts, refractive errors, glaucoma, or macular degeneration.
 Sudden blurry vision in both eyes can be alarming, and it’s a sign that something needs your attention. While not every cause is dangerous, some can pose a serious threat to your vision and overall health.
Sudden blurry vision in both eyes can be alarming, and it’s a sign that something needs your attention. While not every cause is dangerous, some can pose a serious threat to your vision and overall health.

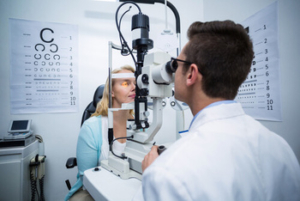
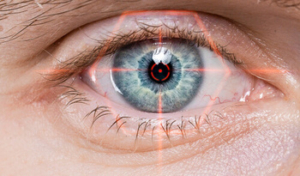 Blurry vision in one eye can feel disorienting, but it doesn’t have to be alarming. The most important thing you can do is listen to your body, notice warning signs, and take action if something doesn’t feel right.
Blurry vision in one eye can feel disorienting, but it doesn’t have to be alarming. The most important thing you can do is listen to your body, notice warning signs, and take action if something doesn’t feel right.
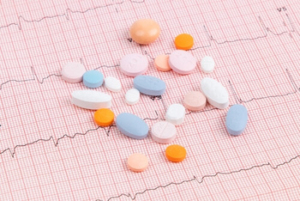 Originally used to treat your heart and blood vessels and manage things like chest pain and even stage fright, these medications work by blocking the effects of adrenaline on your body’s beta receptors, also called β-receptors. These tiny sites are found in the heart, blood vessels, lungs, and yes, even your eyes.
Originally used to treat your heart and blood vessels and manage things like chest pain and even stage fright, these medications work by blocking the effects of adrenaline on your body’s beta receptors, also called β-receptors. These tiny sites are found in the heart, blood vessels, lungs, and yes, even your eyes. Like all medications, beta blockers
Like all medications, beta blockers Whether you’re managing your IOP or seeking more information, it’s always best to speak with a qualified professional who can guide you with knowledge and care.
Whether you’re managing your IOP or seeking more information, it’s always best to speak with a qualified professional who can guide you with knowledge and care.
 ICL eye surgery is a type of refractive surgery that involves
ICL eye surgery is a type of refractive surgery that involves Here’s what you can expect:
Here’s what you can expect: Every eye is unique. The best way to know whether you’re a candidate for this advanced form of refractive surgery is to book an initial consultation with an experienced and appropriately qualified health practitioner.
Every eye is unique. The best way to know whether you’re a candidate for this advanced form of refractive surgery is to book an initial consultation with an experienced and appropriately qualified health practitioner.